Advanced Neuro Surgery & Neurology Care at Shri Jagannath Charitable Cancer Hospital
A small delay in treating neurological problems can lead to serious, life-altering complications. Whether it’s a persistent headache, sudden weakness, or vision issues, these symptoms should never be ignored.
If you are searching for a good neurologist near me, a trusted neuro hospital near me, or the best neuro surgeon in Delhi NCR, choosing the right hospital can make all the difference between delayed recovery and a successful outcome.
Shri Jagannath Charitable Cancer Hospital is committed to providing advanced neuro surgery and neurology care with a strong focus on affordability, accuracy, and compassionate treatment. Trusted by patients across Delhi NCR, Noida, Ghaziabad, Faridabad, and nearby regions, the hospital combines modern technology with expert medical care.
Why Neurological Care is More Important Than Ever
Neurological disorders are rapidly increasing due to modern lifestyle, stress, and aging. According to the World Health Organization, neurological conditions affect 1 in 3 people globally.
Key Statistics:
- Over 30 million people in India suffer from neurological disorders
- Stroke cases are increasing every year
Early diagnosis and expert neuro surgery can significantly improve recovery and save lives.
Expert Neuro Surgery with Proven Results
Neuro surgery requires extreme precision, advanced tools, and highly experienced surgeons.
At Shri Jagannath Charitable Cancer Hospital:
- 1000+ successful neurological procedures
- Experienced neurosurgeons with years of clinical expertise
- Advanced operation theatres with modern technology
Conditions Treated:
- Brain tumors
- Spine disorders
- Head injuries
- Nerve-related conditions
Patients searching for the best neuro surgeon in Delhi NCR trust the hospital for its high success rate and patient safety standards.
Find a Good Neurologist Near You
Searching for a good neurologist near me can be confusing. What truly matters is experience, diagnosis accuracy, and patient care.
Why Patients Trust This Hospital:
- Detailed consultations with expert neurologists
- Advanced MRI, CT scan, and diagnostic tools
- Personalized treatment plans
Doctors focus on treating the root cause, not just symptoms—ensuring long-term recovery.
Specialized Neuro Ophthalmology Care
Not all vision problems are eye-related—many are linked to the brain.
The hospital’s neuro ophthalmology services treat:
- Optic nerve disorders
- Double vision
- Vision loss due to neurological conditions
- Eye movement disorders
This multidisciplinary approach ensures accurate diagnosis and faster healing.
Trusted Neuro Hospital Near You in Delhi NCR
If you are looking for a neuro hospital near me, Shri Jagannath Charitable Cancer Hospital stands out for its accessibility and affordability.
Facilities Include:
- Advanced MRI & CT scan
- Emergency neuro care
- ICU for critical patients
- 24/7 medical support
Patients from Delhi, Noida, Ghaziabad, and Faridabad choose this hospital for reliable care.
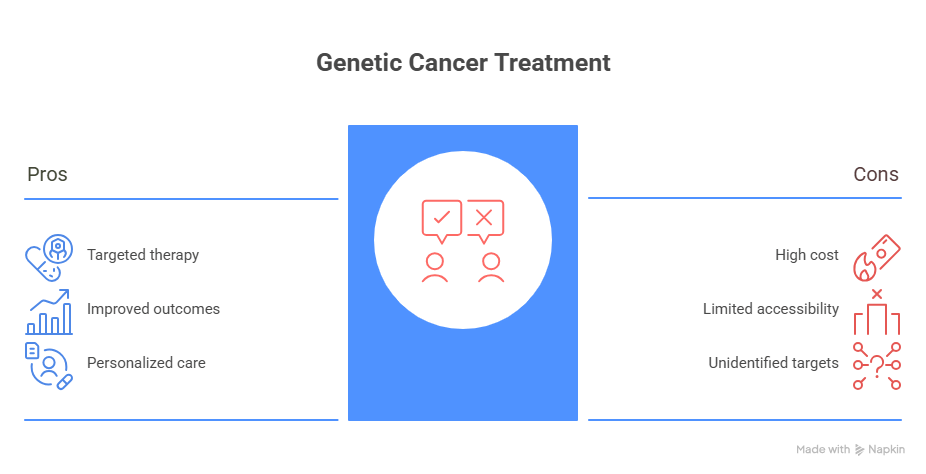
Best Cancer Hospital in Delhi NCR with Neuro Expertise
Shri Jagannath Charitable Cancer Hospital is also recognized among the best cancer hospitals in Delhi NCR, especially for brain and spine-related cancers.
Specialized Treatment:
- Brain tumors
- Spinal cancers
- Cancer-related neurological complications
The integration of oncology and neurology ensures complete treatment under one roof.
Neurophysiotherapy for Faster Recovery
Recovery is a critical phase after neurological treatment. The hospital provides expert neurophysiotherapy to help patients regain independence.
Benefits:
- Faster recovery after stroke or surgery
- Improved mobility and coordination
- Better quality of life
Each rehabilitation plan is customized, ensuring effective and long-term results.
Affordable Treatment with Government Schemes
High-quality treatment should not be expensive. The hospital is committed to providing the best affordable neuro surgery in Delhi NCR.
Government Schemes Available:
- Ayushman Bharat Yojana – Cashless treatment for eligible patients
- Central Government Health Scheme (CGHS) – Coverage for central government employees
Insurance & TPA Support:
- Medi Assist
- Cholamandalam MS General Insurance
- HDFC ERGO
- Niva Bupa
- Universal Sompo
- SBI General
- Star Health Insurance
This ensures cashless, stress-free treatment for patients.
Best Affordable Neuro Surgery in Delhi NCR
Unlike expensive private hospitals, Shri Jagannath Charitable Cancer Hospital focuses on:
- Transparent pricing
- No hidden costs
- Financial assistance options
- High-quality treatment at lower cost
This makes it a top choice for patients searching for:
- Best neuro surgeon in Delhi NCR
- Good neurologist near me
- Neuro hospital near me
When Should You Visit a Neurologist?
Seek immediate medical attention if you experience:
- Frequent or severe headaches
- Memory loss or confusion
- Vision problems
- Seizures
- Weakness or numbness
Early treatment can prevent serious complications and improve recovery chances.
Why Patients Trust This Hospital
Experience: 1000+ successful neuro procedures
Expertise: Skilled neurologists and neurosurgeons
Authoritativeness: Advanced technology & global standards
Trustworthiness: Affordable care with government schemes
FAQs
The best neuro surgeon is one with proven experience, modern surgical techniques, and high success rates. Shri Jagannath Charitable Cancer Hospital offers expert neurosurgeons trusted across Delhi NCR.
Yes, this hospital provides affordable neuro surgery with support from government schemes like Ayushman Bharat Yojana and CGHS.
Look for hospitals with experienced doctors, advanced diagnostics, and strong patient trust—like Shri Jagannath Charitable Cancer Hospital.
Yes, the hospital is empanelled with multiple TPAs like Medi Assist , Chola MS, Star Health Insurance, HDFC ERGO, Niva Bupa, Universal Sompo, SBI General,offering cashless treatment options.
Neurophysiotherapy helps patients recover from stroke, paralysis, and neurological injuries through guided rehabilitation.
Book Your Consultation Today
Don’t ignore early signs of neurological problems. Timely treatment can save lives and prevent complications.
Visit Shri Jagannath Charitable Cancer Hospital today for expert consultation
Get access to the best neuro surgeon in Delhi NCR
Experience affordable, advanced neuro surgery and care
Final Thoughts
Whether you need neuro surgery, are searching for a good neurologist near me, or want treatment at the best cancer hospital in Delhi NCR, choosing the right hospital is critical.
Shri Jagannath Charitable Cancer Hospital offers a perfect combination of expertise, affordability, and compassionate care, making it one of the most trusted healthcare providers in Delhi NCR.
Home > Neurology > Neuro Surgery > Shri Jagannath Charitable Cancer Hospital